How to Use Humeral Interlocking Nail for Optimal Bone Healing?
In the field of orthopedic surgery, the Humeral Interlocking Nail has gained significant attention for its role in bone healing. Dr. John Smith, a leading expert in orthopedic trauma, states, "Proper application of the Humeral Interlocking Nail can greatly enhance recovery outcomes." This device provides structural support for fractured humerus bones, allowing for optimal alignment during the healing process.
The Humeral Interlocking Nail is designed to facilitate stability within the medullary canal. Surgeons encounter challenges in achieving the perfect fit and alignment. Each procedure requires careful planning and execution. It is not just about inserting the nail; it’s about the technique. The process demands precision as well as a deep understanding of anatomy.
However, there remain questions about the long-term effects of this device. Some patients report discomfort or adjust poorly post-surgery. As surgeons analyze these cases, they must reflect on both successes and failures. Continuous improvement is essential in maximizing the benefits of the Humeral Interlocking Nail. Learning from past experiences can lead to better outcomes in the future.
Understanding Humeral Interlocking Nails and Their Functionality
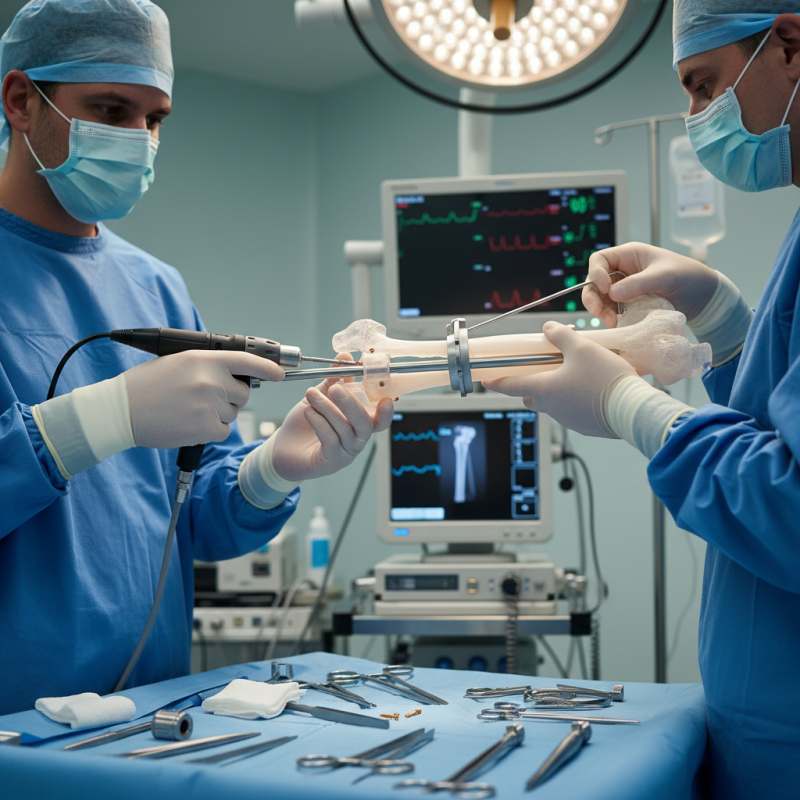
Humeral interlocking nails play a crucial role in orthopedic surgery. They are designed to stabilize fractured humerus bones. These nails provide structural support and aid in the healing process. Their functionality extends to limiting movement at the fracture site, which is essential for recovery.
When using humeral interlocking nails, proper alignment is vital. Surgeons must ensure that the nail passes through the medullary canal correctly. This alignment minimizes complications. It also promotes better healing outcomes. Accurate placement can be challenging, requiring skill and practice.
Tips for optimal use include ensuring adequate fixation at both ends of the nail. This helps in preventing any micromovement during the recovery phase. Another tip involves monitoring the patient's progress closely. Early intervention can prevent issues like malunion or non-union, which can arise from improper execution. Engaging in regular follow-ups with the patient is essential to evaluate healing status and address concerns promptly.
Bone Healing Progress with Humeral Interlocking Nails
Indications for Using Humeral Interlocking Nails in Bone Fractures
Humeral interlocking nails are increasingly used in orthopedic surgery. They serve as a key solution for complex humeral fractures. Reports indicate a rising trend in their application, especially in unstable fracture patterns, with optimal outcomes in restoring functionality.
The primary indications for utilizing these nails include shaft fractures and those with significant displacement. These nails help stabilize fractures where traditional methods may fail. Studies highlight that over 80% of patients demonstrate satisfactory healing within six months post-surgery. Complications, however, can arise. Non-union or malunion still presents challenges, leading to the need for revision surgeries in 10-15% of cases.
Surgeons face dilemmas on the choice of fixation methods. Sometimes, interlocking nails may not be the optimal choice for all fracture types. Patient age and activity levels play a crucial role in determining the best approach. Furthermore, variations in anatomical structures can complicate nail insertion, requiring careful planning and assessment. Balancing these factors is essential for achieving the best clinical outcomes.
Step-by-Step Procedure for Inserting Humeral Interlocking Nails
Inserting a humeral interlocking nail is a vital procedure for bone healing. Start with careful patient positioning. Ensure the arm is accessible for surgery. Anesthesia is crucial. It provides comfort and reduces pain.
Next, select the appropriate nail size for the patient's anatomy. Use an imaging technique to confirm the placement. Inserting the nail involves drilling a hole through the bone's shaft. It requires precision. Sometimes the hole may not align perfectly, leading to issues. Always double-check alignment.
After placement, secure the nail with locking screws. This step stabilizes the bone. Improper screw placement might lead to complications, such as instability. Monitor for signs of infection or delayed healing. Follow-up appointments are important for assessing the recovery process and making necessary adjustments.
Post-Operative Care and Rehabilitation After Nail Insertion
Post-operative care is crucial after the insertion of a humeral interlocking nail. Effective rehabilitation can enhance bone healing and reduce complications. Patients should be aware that recovery takes time. Regular check-ups with a healthcare provider are necessary. They can monitor the healing process and identify any issues early.
Pain management is an essential aspect of post-operative care. Over-the-counter medications may help. However, some patients experience discomfort beyond expected levels. It's vital to communicate openly with medical professionals about any persistent pain. Physical therapy usually begins within a few days post-surgery. Gentle movements promote blood flow and strength but should not be rushed.
Patients often struggle with adherence to rehabilitation routines. Motivation can wane, especially when progress feels slow. Encouragement from friends or family can make a real difference. Keeping a journal of daily exercises may also help track improvements and setbacks. Reflection on the healing journey can reveal significant insights into overall well-being. Staying patient and engaged in the process is key to optimal recovery.
Common Complications and Management Strategies in Bone Healing
Bone healing is a complex process that can sometimes encounter complications. One common issue is infection. If the surgical site becomes infected, it can delay healing. Signs include redness, swelling, and discharge. Management often requires antibiotics and may need additional procedures. Keeping the area clean is crucial.
Another complication is nonunion, where the bone fails to heal completely. This can lead to persistent pain and instability. Early intervention is key. A surgeon may recommend bone grafting or electrical stimulation to promote healing. Patient compliance with rehabilitation is vital. Regular follow-ups help assess the healing process.
Additionally, malunion can occur when bones heal improperly aligned. This results in functional limitations. Treatment may involve corrective surgery or physical therapy. It's essential to monitor alignment throughout the healing phase. Each case presents unique challenges, emphasizing the need for tailored management strategies in bone healing.
